Revenue Cycle Excellence
Generic RCM solutions leave revenue exposed. Our single-specialty expertise, performance data, clinical documentation improvement, and managed care integration strengthen documentation integrity, reduce revenue leakage, and drive consistently higher collections.
Why is anesthesia revenue cycle management so complex?
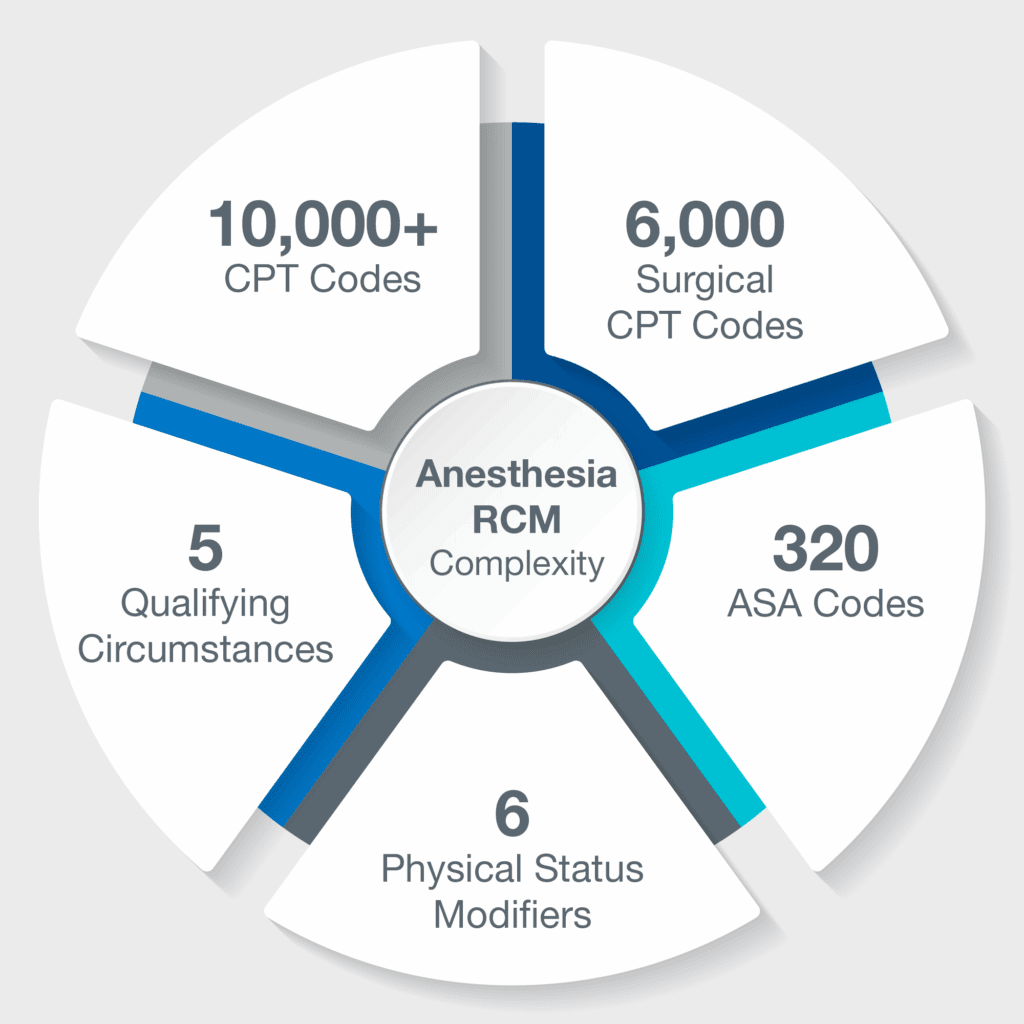
Unlike other medical specialties that bill by procedure type alone, the cost for anesthesia services depends on several factors tied billing codes and modifiers determined by the American Society of Anesthesiologists. When an revenue cycle management (RCM) team fails to manage these factors effectively, hospitals and health systems face lost reimbursement, reduced revenue, compliance risks, and patient dissatisfaction.
Anesthesia reimbursement depends on precise, time-based coding that captures exact start and stop times for every case. Each record must document who provided care, how it was supervised, and the applicable modifiers. These factors can vary by payer, state, and clinical structure. When medical direction or concurrency is involved, the complexity multiplies. Without an anesthesia-specific RCM system, billing teams can struggle to maintain accuracy and compliance. NAPA’s model streamlines this process with structured documentation and ongoing audits to ensure revenue integrity.
Our RCM Competitive Advantage
By focusing exclusively on anesthesia’s unique challenges, our end-to-end RCM engine drives operational excellence, helping practices achieve superior financial outcomes while working to maintain compliance and efficiency across the board.

Days in A/R
34*
U.S. Avg: 50.7

Annual Net Collections
96.7%*
U.S. Avg: 86.8%

Initial Denials
8.3%*
U.S. Avg: 13.8%
*Past performance does not guarantee future results. Each client’s experience is dependent on unique factors.
NAPA’s RCM process follows the standard stages of revenue management, from the moment a bill is created to the moment it is paid. While NAPA successfully achieves each stage of the process, we excel in ones that matter most, specifically front-end reconciliation and registration, billing and claim submission, clinical documentation improvement and revenue optimization, and patient responsibility. We prioritize onshore billing operations, thereby working to deliver greater transparency and security for our partners and patients.
An End-to-End RCM Process
Our service involves the seven main stages of revenue cycle, beginning on day-of-service accounting and ending with final payments. Continuous Clinical Documentation Improvement (CDI) and Revenue Optimization is embedded across our entire process. Our audit teams continuously work to close gaps to uphold compliance and documentation precision, delivering cleaner claims and appropriate, defensible reimbursement.
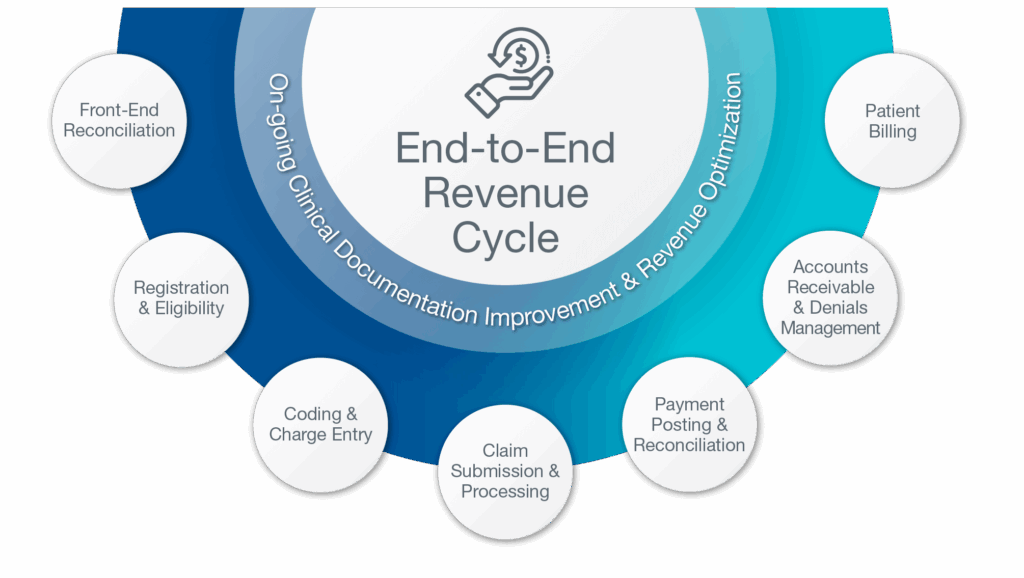
Our system is designed to deliver transparency, accuracy, and speed.
- Front-end Reconciliation: Our streamlined process validates patient and payer information at check-in and check-out to catch discrepancies before claims are created. By confirming real-time eligibility, coverage changes, and required payments, we continuously work to reduce preventable claim rejections.
- Registration & Eligibility: Our workflows verify patient details, including insurance coverage, benefits, deductibles, and any authorizations before the day of service. This can reduce avoidable denials and supports faster, more accurate reimbursement.
- Coding & Charge Entry: Our anesthesia expertise, empowered with AI-driven solutions, delivers cost efficiency and coding precision.
- Claim Submission & Processing: Our advanced platform ensures compliance and flexibility regardless of care team configuration.
- Payment Posting & Reconciliation: Our real-time payments integrate seamlessly and with fewer errors to patient accounts.
- Accounts Receivable & Denials Management: Our automated processes and integrated contract management reduce AR days to fast-track collection without compromising on performance.
- Patient Billing: Our partnership with Cedar’s self-pay platform creates a digital-first financial experience that is simple, transparent, and routinely praised by patients.
How Managed Care Influences Revenue Cycle Management
Managed care and RCM are deeply interconnected. Managed care sets the rules for reimbursement, while RCM provides the systems and expertise to support full value capture of services. When these two functions align, it strengthens financial stability, reduces inefficiencies, and creates a smoother revenue experience for all stakeholders. At NAPA, our highly skilled and experienced managed care and RCM teams routinely collaborate in an effort to maximize value for our partners.
Key Advantages of Integrated Managed Care and RCM
- Financial Strength: Executes managed care contracts effectively to maximize reimbursement and protect revenue
- Expert Navigation: Precisely handles complex payer models
- Operational Efficiency: Automates and streamlines billing while accelerating cash flow and reducing administrative burdens
- Actionable Insights: Leverages data to identify trends, improve claim performance, and guide strategic decisions
- Patient-centered Experience: Simplifies billing and payment processes to improve clarity and satisfaction
- Fewer Denials: Supports more accurate claims and timely payments, limiting errors and minimizing revenue leakage
Contract Clarity on Day One
Our payer configuration team sets the foundation for clean, compliant revenue. We validate every payer contract at onboarding and audit each charge against contracted allowables to avoid undercharging. Payer-specific rules are automated and continuously monitored to maintain all amendments, renewals, and escalators. This protects rate integrity over time and drives cleaner claims, fewer denials, higher capture, daily accuracy, and compliance.
They also account for the details that vary by payer and change frequently: split billing requirements (e.g., anesthesia billed separately from facility or surgeon), precise modifier usage (service type, provider type, patient status, medical direction), time caps for extended-duration care such as OB, and contract-defined conversion calculations by payer, location, and current year. Missing these nuances hurts yield.
Leading Reimbursement through Independent Dispute Resolution

Since the No Surprises Act (NSA) went into effect in 2022, anesthesia reimbursement has faced an uphill struggle with commercial payers. Navigating this challenge requires the combined strength of managed care expertise and RCM excellence to safeguard predictable commercial revenue and avoid:
- Payer underpayments
- Administrative delays
- Financial instability risk
- Patient confusion and frustration
The NSA created a new process for resolving out-of-network payment debates called Independent Dispute Resolution (IDR). NAPA enacted a powerful strategy that has achieved exceptional outcomes. These results reinforce NAPA’s role as an industry leader in ensuring fair, equitable reimbursement while protecting patients from financial harm.

