5 Things Healthcare Leaders Should Know About Anesthesia Revenue Cycle Management
By Lynn Van Houten, SVP, Revenue Cycle Management, NAPA
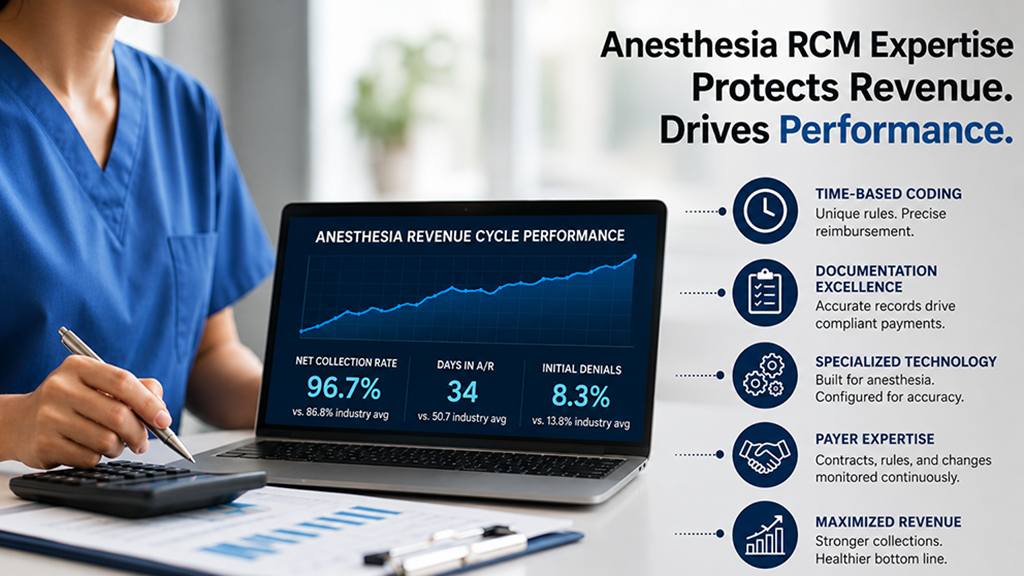
Why anesthesia RCM expertise is the difference between protected revenue and preventable loss
Anesthesia revenue cycle management (RCM) is one of the most misunderstood areas of healthcare finance. Many organizations expect anesthesia billing to function like other specialties. It does not. And when anesthesia RCM is managed without deep specialty expertise, organizations face increased risk of underpayments, compliance exposure, preventable denials, and significant revenue leakage.
Unlike traditional medical billing, anesthesia operates in a highly specialized environment driven by time-based coding, payer-specific modifiers, concurrency calculations, medical direction requirements, and rapidly evolving reimbursement rules. Non-specialized RCM processes (or broad-based billing vendors) often miss the nuances that directly impact reimbursement performance.
For hospitals and health systems, the question is no longer whether anesthesia revenue is complex. The question is whether your current RCM infrastructure truly understands how to protect it.
Here are five things every healthcare organization should know about anesthesia RCM and what’s at risk without specialized expertise.
1. Anesthesia Billing Is More Than a Unit Rate
Anesthesia billing is fundamentally different from most medical specialties and requires deep operational and coding expertise beyond a standard CPT-based reimbursement model. Reimbursement is not determined solely by a unit rate calculation. It depends on:
- Precise start and stop times
- ASA-specific coding
- Modifier application
- Concurrency calculations
- Medical direction requirements
- Highly detailed documentation standards
Even payer reimbursement methodologies vary significantly, with some carriers reimbursing in 10-minute increments while others apply 12- or 15-minute rounding methodologies.
This complexity creates substantial financial and compliance risk for organizations relying on generalized billing teams or non-specialized RCM platforms. Small documentation gaps, incorrect modifier usage, or inaccurate concurrency reporting can materially impact reimbursement, increase denial rates, or create compliance exposure. Concurrency management alone, which determines how many cases an anesthesiologist supervises simultaneously, directly affects both billing methodology and reimbursement outcomes.
Unlike traditional physician billing, anesthesia RCM requires specialty-specific expertise to accurately capture reimbursement, maintain compliance, and minimize revenue leakage.
2. Clinical Documentation Directly Impacts Revenue Integrity
In anesthesia, documentation is not just a clinical record. It is the foundation for compliant reimbursement.
Medical direction requirements depend on highly specific provider attestations and documentation standards. If documentation is incomplete, reimbursement may be reduced even when care was delivered appropriately.
That is why leading anesthesia RCM organizations embed Clinical Documentation Improvement (CDI) directly into the revenue cycle process.
Specialized CDI teams continuously monitor documentation trends, identify deficiencies, educate providers, and optimize electronic medical record workflows to ensure billing accurately reflects the care that was delivered.
Without this type of infrastructure, organizations face two major risks:
- Lost reimbursement from undercoded or unsupported claims
- Increased exposure to audits and compliance scrutiny
The stakes are high. A single documentation issue repeated across thousands of cases can create substantial financial impact over time.
3. Most Traditional RCM Platforms Were Not Built for Anesthesia
Many health systems rely on enterprise billing systems designed for broad physician services. The problem is those platforms often cannot manage anesthesia’s unique requirements without significant customization.
Concurrency calculations, split billing, modifier logic, academic medical center workflows, and payer-specific anesthesia rules require specialized functionality that many systems simply do not support.
The anesthesia-specific workflows developed by NAPA for our clinical services clients, and additionally provided to our managed services partners, are embedded directly into the platform architecture. The system begins working as soon as a patient is scheduled, which eliminates common delays and improves billing accuracy from the outset.
That infrastructure advantage matters.
NAPA’s anesthesia-focused RCM performance includes:
- Days in A/R of 34 (compared to a U.S. average of 50.7)
- Net collections of 96.7% (compared to an industry average of 86.8%)
- Initial denials of only 8.3% (compared to an industry average of 13.8%)
Those results are not accidental. They come from a system purpose-built for anesthesia.
4. Managed Care and RCM Must Work Together
One of the biggest gaps in anesthesia reimbursement occurs when managed care contracting and RCM operations operate independently.
Every payer contract contains unique billing rules, modifier requirements, conversion factors, and reimbursement methodologies. If those rules are not correctly interpreted and configured into the billing system, organizations can experience systematic underpayments without detecting them.
This is where anesthesia expertise becomes critical.
Leading anesthesia RCM organizations continuously monitor payer policy changes, validate contract configurations, audit reimbursement variances, and proactively identify discrepancies before they become long-term financial problems.
Without that level of oversight, revenue leakage can occur quietly over months or years.
5. The Financial Impact of Missed Payer Changes Can Be Massive
Perhaps the clearest example of anesthesia RCM complexity is how quickly payer rule changes can create multimillion-dollar exposure.
In one case, a large health system overlooked a major insurer’s anesthesia billing guideline update involving modifier recognition and medical direction reporting. As a result, the insurer failed to reimburse approximately 50% of anesthesia claims.
NAPA’s anesthesia-specific RCM infrastructure immediately identified the reimbursement variance. The team analyzed the data, validated the payer discrepancy, and partnered with the health system to pursue corrective action. The outcome: reversal of the insurer’s decision and recovery of more than $13 million in current and retroactive reimbursements.
That kind of financial recovery does not happen through generic billing oversight. It is the result of unmatched anesthesia expertise, advanced analytics, continuous auditing, and industry-expert teams that understand the evolving payer landscape at a granular level.
The Bottom Line
Anesthesia services are too financially important to surgical services and too financially complex to manage with generalized revenue cycle strategies. Your anesthesia revenue cycle is not just a billing function. It is a financial asset that requires specialty-specific expertise to perform at the highest level.
The real question healthcare leaders should ask is simple: Does your current anesthesia RCM model truly understand anesthesia well enough to protect every dollar your organization has earned?
Lynn Van Houten leads one of the nation’s most advanced anesthesia revenue cycle operations, overseeing performance across 26 states and a team of more than 540 specialists managing the full RCM lifecycle. Under her leadership, NAPA’s RCM engine consistently outperforms industry benchmarks in key metrics such as net collections, days in A/R, and denial rates, driving stronger, more predictable financial outcomes for healthcare organizations. With more than 26 years of experience, Lynn is known for turning complex revenue cycle environments into high-performing, data-driven operations. She has led large-scale transformations across health systems, physician groups, and national RCM organizations, unlocking millions in previously missed revenue, accelerating cash flow, and strengthening compliance in highly regulated environments.
