Blog: How anesthesia grew critical care services during COVID-19

By Cheryl Cranick, Copywriter/Editor, North American Partners in Anesthesia (NAPA)
When COVID-19 struck the U.S. and elective surgeries were halted, anesthesia professionals were called upon to expand critical care teams and help battle this healthcare crisis. Practices across the U.S. shifted gears and readied for a local influx of COVID-19 patients. As the virus tore through New Jersey and the New York metro area, 60 of our clinicians from across the country raised their hands and traveled to this COVID-19 hot zone, serving on code and intubation teams or within intensive care units (ICUs).
With COVID-19 cases spreading across our country, New Jersey was not unique in its initial COVID-19 response. Anesthesiology practices throughout the country prepared with their health systems and set up operating and recovery rooms as overflow ICUs. They leveraged relationships to secure additional ventilators or transitioned anesthesia machines to serve as ventilators, trained with personal protective equipment (PPE), and waited for a surge. Where New Jersey differed was its overwhelming need for this preparation, as hospitals were rapidly inundated with COVID-positive patients.
Why anesthesia
Anesthesia healthcare professions have unique skills and experience that proved critical in this pandemic. They are experts in ventilator and airway management, complex hemodynamic management and instability, respiratory failure, and invasive monitoring. Anesthesiologists are trained in critical care, and nurse anesthetists typically come from a critical care nursing background. Still, COVID-19 was a virus nearly impossible to fight.
“This pandemic was unlike anything I have seen in my time as a physician,” said Daryl Fenio, MD, an anesthesiologist from Reno, NV, who spent more than a month in New Jersey. “As a doctor, I’ve seen all the problems COVID-19 brought, but not in these numbers or strange combinations. These patients were on complicated regimens — drug and ventilator managements unlike what most of us typically deal with, instability of blood pressure, inability to oxygenate, multi-organ system failure, and novel drug treatments, with recommendations changing daily.”
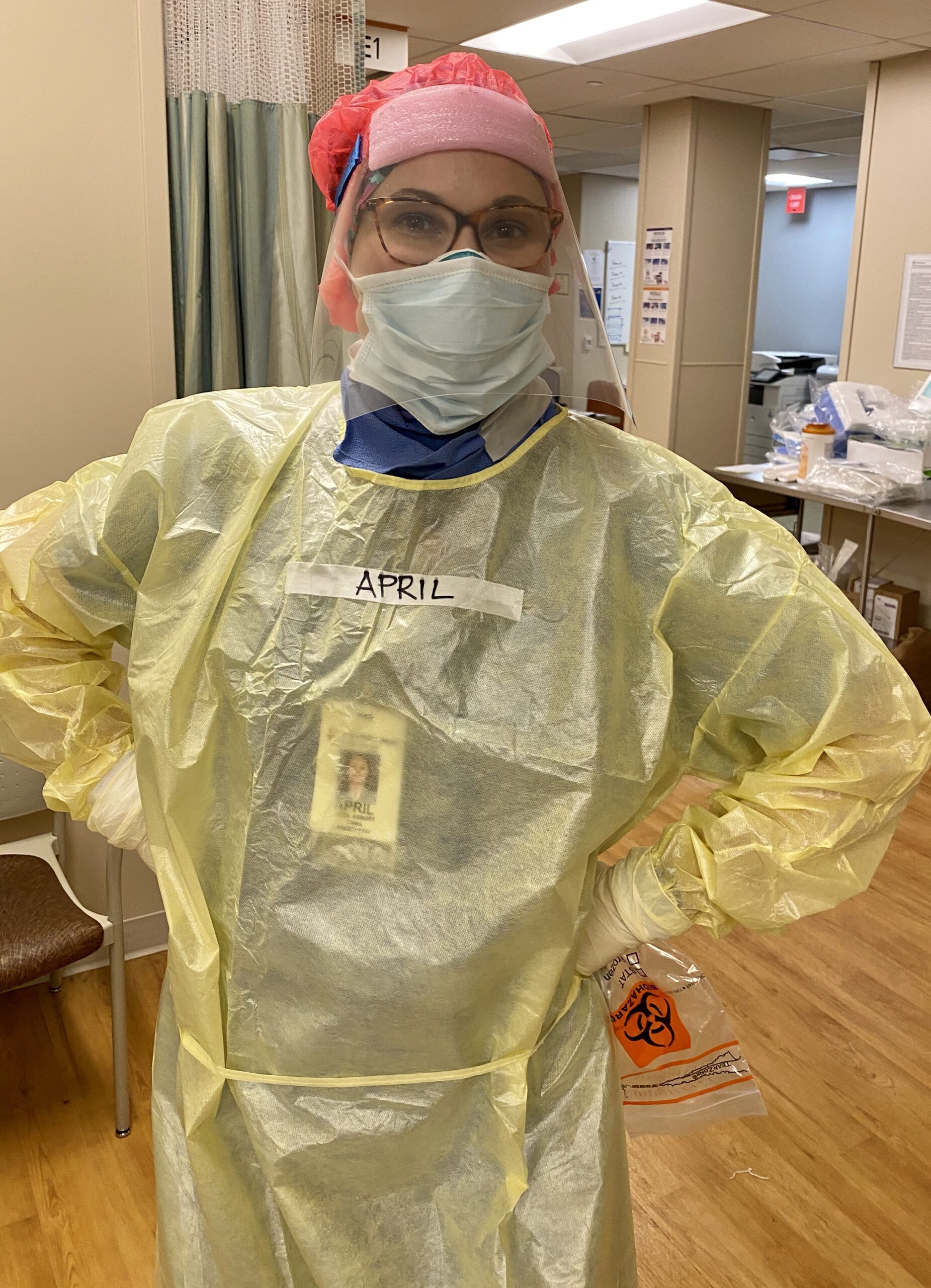
Serving at the COVID front lines
Understanding the critical role they could play in New Jersey, dozens of anesthesiologists and certified registered nurse anesthetists (CRNAs) answered the call to mobilize. These clinicians jumped into the fight, working alongside unfamiliar colleagues in unfamiliar environments for exhausting 12-hour shifts. They traveled to New Jersey knowing they would step into health facilities overcome by this virus — a virus that was winning against modern medicine.
“For me, the bottom line was fear could not define my decision,” said Nick Keene, CRNA, from Richmond, VA, who joined a code and intubation team in New Jersey. The experience was not without its dark moments. The extreme loss of life “weighed heavy on my mind” he said. “Usually in anesthesia, if we experience a crisis, we can manage it, and for the most part have a good outcome,” he said. “COVID was different, and I had to mentally prepare myself each day.”
To prevent further spread of the virus, family members were unable to be with their loved ones, even as they passed. For anesthesia professionals, this was a new and emotional experience. “The degree of social isolation brought on by this pandemic was extreme,” said Leslie Walton, DO, MBA, from Warren, MI. “I came to understand I was the lifeline between patients and families. I was the only way families knew of their loved one’s status.”
April Asbury, CRNA, also from Richmond, supported roughly 15 COVID-positive patients or more at any given time in a transformed COVID wing. Like her colleagues, she tried to remain positive. “I was thankful to serve the people of New Jersey — the nurses and the doctors as much as the patients,” she said.

Communication and teamwork remained essential during this time. “I became a much better listener as a result of this experience,” said Katherine Hopper, DNAP, CRNA, another Richmond clinician. “If a nurse had a concern or unique opinion, I took the time to understand it. If a respiratory therapist had a suggestion for an alternative ventilation mode, I would carefully hear the input. If intensivists and pharmacists had differing thoughts about therapeutic versus prophylactic anticoagulation, I would weigh the pros and cons of each side. No one-size-fits-all rule applied to COVID’s wrath. We had to analyze, observe, and listen to every little detail to create a safe plan of care for each patient.”
Providing this critical care to thousands of New Jersey patients, healthcare colleagues, and hospital partners was noble and important work. “I went there to learn, to see and do, and to help our sisters and brothers in anesthesia,” said Isaiah Fuller, CRNA, from Memphis, TN. “But seeing it firsthand, nothing could have prepared you.”
We remain grateful and honored to have such a dedicated team of anesthesia clinicians across our broad network, who applied their expertise, their ingenuity, their energy, and their dedication to patient care throughout this healthcare crisis. We take this moment to specifically recognize the 60 clinicians who left their home sites and worked side-by-side with our teams and patients in New Jersey:
Margaret Allen, CRNA (GA)
James Anderson, CRNA (VA)
April Asbury, CRNA (VA)
Mehtab Bajwa,
MD (NY)
Sabrina Bent, MD (Regional)
Aja Bjerke, MD (NV)
Daniel Chang, CRNA (NY)
Meghan Nicole Chupick,
CRNA (VA)
Sarah Chism, CRNA (GA)
Eliyahu Cooper, MD (Regional)
Chelsea Coscarelli, CRNA (VA)
Anne
Cousins, CRNA (VA)
Timothy Dowd, MD (Regional)
Paul Evelyn, CRNA (GA)
Daryl Fenio, MD (NV)
Isaiah
Fuller, CRNA (TN)
Catherine Gabel, CRNA (TX)
Robert Gardner, CRNA (TN)
Jeffrey Gladding, MD
(NV)
Benjamin Griffin, CRNA (TN)
Daniel Hansen, MD (NV)
Kathleen Harden, CRNA (NY)
Tessa Hartmann, CRNA
(VA)
Robert Hooko, CRNA (NY)
Katherine Hopper, DNAP, CRNA (VA)
Shanericka Jones, CRNA (VA)
Nicholas
Keene, CRNA (VA)
Kevin Kolodgie, CRNA (VA)
Curry Lee, CRNA (TN)
Mark Lipkind, MD (Regional)
Josephine Low, CRNA (TN)
Tenaja Lynch, CRNA (VA)
Kathryn Jaye Martin, CRNA (VA)
Morgan
McCarroll, MD (NV)
James McLeod, DNAP, CRNA (GA)
David Milek, MD (MI)
Ann Marie Mullen, CRNA
(PA)
Shannon Nelson, CRNA (TN)
Hazel Pickering-Luttrell, CRNA (VA)
Jessica Ray, CRNA (VA)
Nariman
Rahimzadeh, MD (NV)
Tony Randazzo, MD (NJ)
Delia Rhinehart, CRNA (TN)
Gretchen Ritter, CRNA (VA)
Kristen
Ryder, CRNA (NY)
Jennifer Schofield, CRNA (VA)
Rivka Ariella Schwarcz, CRNA (VA)
Kofi Sey, CRNA
(VA)
Kevin Smith, CRNA (TN)
Tavya Sprat, CRNA (VA)
Joseph Staggenborg, MD (Regional)
Andrew Stufflebean,
CRNA (GA)
Alexandra Porter Taylor, CRNA (VA)
Mark Troendle, CRNA (NY)
Shanice Tucker, CRNA (NY)
Ashley
Vacca, CRNA (TN)
Tracy Walker, CRNA (TN)
Leslie Walton, DO (MI)
Brett Winthrop, MD (NV)
Daniel Zauski,
CRNA (NY)
This list represents clinicians from North American Partners in Anesthesia (NAPA) and American Anesthesiology. In May 2020, NAPA acquired American Anesthesiology. Together, we now provide care for three million patients annually at 500 healthcare facilities in 20 states and the District of Columbia.
