How Scaling Standardized Protocols in a Perioperative Surgical Home Saved One Hospital up to $12 Million in One Year and Improved Surgeon Engagement

© 2025 NAPA Management Services Corporation. All rights reserved.
Overview
At New Hanover Regional Medical Center (NHRMC), a not-for-profit, 850-bed teaching hospital, regional referral center, and Level 2 Trauma Center serving southeastern North Carolina and northeastern South Carolina, a Perioperative Surgical Home (PSH) program piloted in orthopedics saved the hospital $4.2 million in the first year.
Monetizing the PSH efforts through a fair market valuation benefited all the hospital’s stakeholders and, with proof of concept and demonstrated return on investment (ROI), enabled scaling the PSH to encompass 16 service lines that produced an annual ROI of up to $12 million.
Situation
Value-based care delivery is dependent on perioperative value. Approximately 45% to 60% of a hospital’s revenue and expenses are related to perioperative services, and bundled payment models demand standardization and reliability to be successful.
Yet at many hospitals, high variability in outcomes and costs—attributed to inconsistent methodologies across the spectrum of care—produces a misalignment of goals among physicians, staff, and administrators. Besides delayed cases, slow OR throughput, and dissatisfied surgeons, significant deviations between same procedures performed by different surgeons inhibit organizations from offering competitive pricing or assuming the financial risk of managing community health.
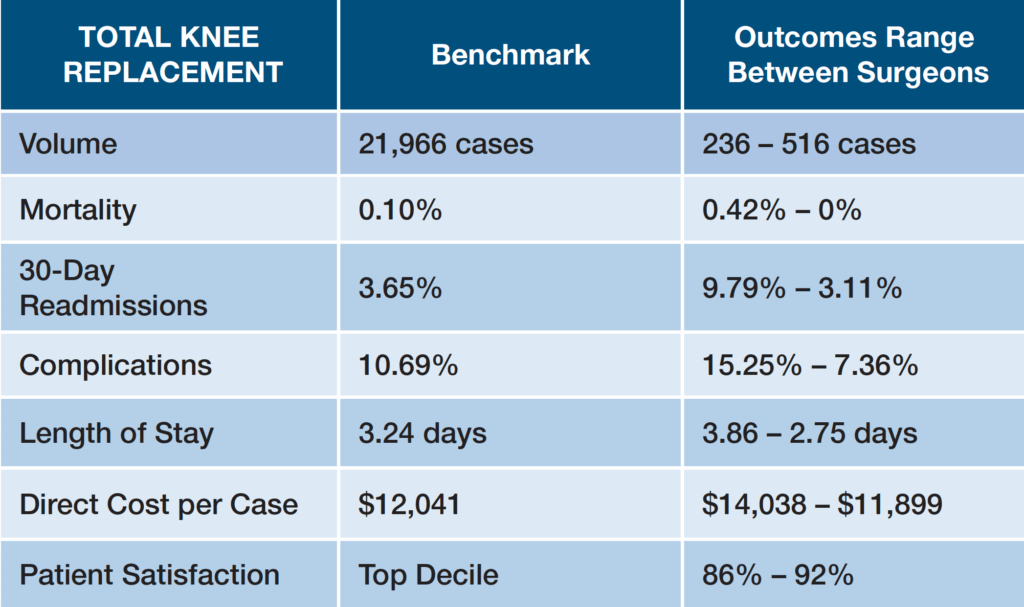
This was the case in NHRMC’s total joint program, where a wide variation in reported metrics for two surgeons highlighted the need for standardized perioperative processes. Compounding the financial impact of case cancellations, inefficient OR scheduling, and unnecessary clinical interventions, CMS readmission penalties in orthopedics alone were costing the hospital approximately $1 million per year.
Solution
The anesthesia department, interacting with every phase of patient care, is uniquely positioned to build stakeholder alignment and effect systemic change. At NHRMC, the Chief of Anesthesia and a dedicated Nurse Navigator championed the PSH concept collaboratively to demonstrate how it could reduce net costs and drive value. Seeking a way to solve for approximately $1 million in readmission penalties, hospital leaders agreed to pilot a PSH in the orthopedics service line.
Building the program began with a lean process that brought all the stakeholders together. The Chief of Anesthesia became Chair of PSH, overseeing PSH leadership comprising anesthesia and surgery management teams supported by nursing, human resources, social services, information technology, pharmacy, laboratory, central supply, and radiology microsystems. Implementation included initiatives across the care continuum, with broad buy-in for measures that had decisive impacts on patients, surgeons, efficiency, and profitability:
- Partnered with hospitalists to institute patient-centered, standardized, evidence-based care, including ERAS protocols, from pre-op through intraoperative, post-op, and post-discharge recovery
- Partnered with a Nurse Navigator to manage patients’ end-to-end experience within the PSH
- Established an anemia clinic in the pre-admission testing (PAT) clinic as part of the risk assessment analysis process
- Created a risk assessment tool to identify patients likely to be readmitted
- Increased patients’ pre-surgical preparation period from 3 to 21 days to ensure operative health eligibility and reduce case delays and day-of-surgery cancellations
- Connected case managers to patients in pre-testing; conducted cognitive and frailty assessments and post-surgery patient education, including home visits by paramedics
- Gained surgeon agreement to standardize lab order-sets for specific procedures, which reduced variation and decreased costs
- Created a transitional care clinic to provide post-surgical medical oversight
- Benchmarked performance and cost metrics and shared data analytics transparently
- Engaged surgeons and anesthesiologists in co-management agreements that provided fair market value compensation incentives for meeting targeted service-line and OR metrics
Results
A Standard Methodology Translates to Fiscal Success
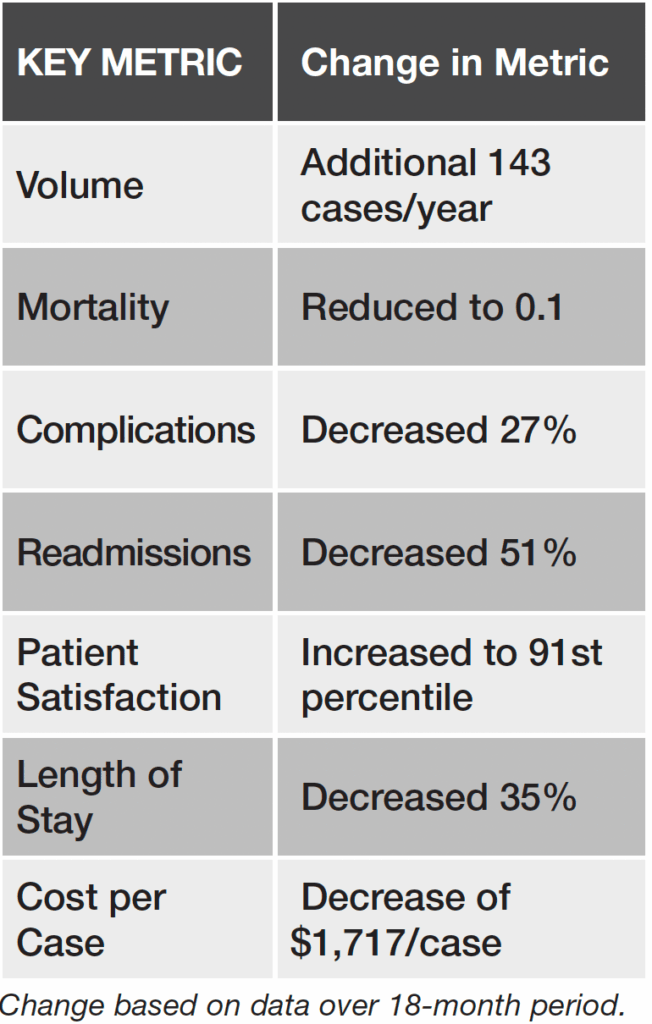
The hospital C-suite and surgeons across other specialties soon noticed the value driven by the total joint PSH. With more efficient case and staff scheduling, first case on-time starts rose from 65% to the top decile. OR utilization increased to 92%, while surgeons’ overtime decreased. A substantial drop in blood transfusion rates saved $800,000.
After the first year, the lowest-performing surgeon achieved outcomes at the highest-performing levels of comparable total hip/knee centers. As outcomes improved, so did patient satisfaction scores, which rose to the 92nd to 95th percentile in every quarter of year one.
Led by anesthesia, the PSH team was acknowledged as patient-focused solution providers who were equally engaged in decreasing operational costs. PSH adds value by aligning hospital strategy with that of high-reliability organizations and promoting clinical leadership and programs that enhance quality and patient safety. In the PSH, patient experience and hospital profitability rise together, earning consumer loyalty and industry recognition. After NHRMC expanded the PSH to 16 service lines, it achieved an annual ROI of up to $12 million, with margins averaging 7% to 8%. PSH was credited with contributing to the strong margins that supported the hospital’s $5.3 billion sale in October 2020.
Let’s Connect: Solutions@napaanesthesia.com | 833-OR1-TEAM